Screening and Vaccination for Cervical Cancer
Cervical cancer is the tenth most common cancer among women in Singapore.* It is however a highly preventable cancer because we are able to catch the precancerous stages caused by the persistent high risk or cancer-causing HPV infection using a very reliable and affordable cervical smear test.
All women between the ages of 25 and 69 years old who have ever had sexual activity are recommended to go for their regular cervical screening as part of the national cervical screening programme.
*Singapore Cancer Registry 2023
How can I protect myself against cervical cancer?
Pap Test
The Papanicolaou test (also sometimes known as a Pap test or a Pap smear) is the examination of cervical cells to detect cell changes that may be early signs of cervical cancer. To get the cells for testing, a doctor or nurse will collect a sample of cells from your cervix that will be sent for testing.
What happens during a Pap Test?
The Pap test is a simple procedure that takes only a few minutes. It can be done in a clinic by a doctor or a nurse.
- During the procedure, the woman being examined lies on her back with her knees drawn up and apart.
- An instrument called a speculum is inserted into the vagina (birth canal) to expose the cervix, which is the lower end or neck of the uterus that extends into and can be seen via the vagina.
- The healthcare professional (doctor or nurse) then uses a small disposable brush or spatula to collect a sample of cells from the outer opening of the cervix. The sample is smeared onto a glass slide or put into a container and sent for analysis.
- After removing the speculum, the healthcare professional performs a pelvic examination by gently inserting two gloved fingers into the woman’s vagina while placing his or her other hand on the woman’s abdomen to check on the size, shape and consistency of the uterus, ovaries, and fallopian tubes.
It is important to remain calm and relaxed during the test. Some women may experience mild discomfort or dull pressure during the Pap test or pelvic examination. However, these procedures should not be painful. Please inform the healthcare professional immediately should you experience any pain.
When will I get the results of my Pap Test?
You will receive your Pap test results 4 to 6 weeks after the test is done. Your Pap test result will indicate whether the smear is normal or abnormal.
Like all screening tests, the Pap test is not perfect. Because the Pap test takes a very small sample of cells present in the cervical area, early cell changes will not be detected if the smear does not contain enough abnormal cells.
It is possible that the Pap test can result in “false positives” and “false negatives”. A false positive incorrectly indicates that there may be cancer when cancer is not present. A false negative incorrectly indicates that all may be normal when a cancer or pre-cancer abnormality is actually present.
Follow-up Actions:
If the results are normal or negative, the laboratory report will be posted to you with an accompanying letter advising you on the date of your next Pap test.
If the results are abnormal or positive, a nurse from the clinic will call you to make a subsequent appointment to either repeat your Pap test or to follow-up with a doctor for further tests.
How often should I go for Pap Test?
The Pap test is for women who have ever had sex.
Women between the ages of 25-29 are recommended to get a Pap test done once every 3 years.
How should I prepare for my Pap Test?
If you are still menstruating, schedule your Pap test appointment 2 weeks after the start of your menstrual period, up to about a week before your next menstrual period is due. This is the ideal time to have a Pap test when the clearest, cleanest sample of cervical cells can be obtained.
If you have reached menopause, you may schedule a Pap test at any time of the month.
Things to avoid:
48 hours before your Pap test, please avoid:
- douching
- swimming
- taking a tub bath
- sexual intercourse
- lubricants
- spermicides
- vaginal creams
- vaginal medications
- tampons
These activities or products can irritate the cervix. Avoiding these activities will help ensure adequate cell sample collection. Other factors that may affect Pap test results include infection and the intake of medication such as digitalis and tetracycline.
What To Wear For Your Appointment
For your Pap test appointment, please wear a two-piece outfit.
It may also be a good idea to bring along a panty liner or thin sanitary pad as light bleeding or spotting may occur after a Pap test.
HPV Test
The Human Papillomavirus (HPV) test is a screening test for cervical cancer. The HPV test analyses a small amount of cells taken from the cervix to detect the presence of the human papillomavirus, a virus that can lead to the development of genital warts, abnormal cervical cells or cervical cancer.
The sampling procedure for a HPV test is carried out in the same way as a Pap test.
What happens during a HPV Test?
It is a simple procedure that takes only a few minutes. It can be done in a clinic by a doctor or a nurse.
- During the procedure, the woman being examined lies on her back with her knees drawn up and apart.
- An instrument called a speculum is inserted into the vagina (birth canal) to expose the cervix, which is the lower end or neck of the uterus that extends into and can be seen via the vagina.
- The healthcare professional (doctor or nurse) then uses a small disposable brush or spatula to collect a sample of cells from the outer opening of the cervix. The sample is then put into a small container and sent to the lab for analysis.
It is important to remain calm and relaxed during the test. Some women may experience mild discomfort or dull pressure during the HPV test. However, these procedures should not be painful. Please inform the healthcare professional immediately should you experience any pain.
When will I get the results of my HPV Test?
You will receive your HPV test results 4 to 6 weeks after the test is done. Your HPV test result will indicate whether the test is positive or negative.
- A negative HPV test means you do not have an HPV type that is linked to cervical cancer.
- A positive HPV test means you have an HPV type that may be linked to cervical cancer. This does not mean you have cervical cancer now. However, it is a sign that cervical cancer could develop later. You will probably be advised to go for follow-up or more tests to monitor and/or diagnose your condition.
Follow-up Actions:
If the results are negative, the laboratory report will be posted to you with an accompanying letter advising you on the date of your next HPV test.
If the results are positive, a staff from the clinic will call you to make a subsequent appointment to either repeat the HPV test / Pap test or to follow-up with a doctor for further tests.
How often should I go for HPV Test?
The HPV test is for women who have ever had sex. Women aged 30 and above are recommended to get a HPV test done once every 5 years.
How should I prepare for my HPV Test?
When To Make An Appointment
If you are still menstruating, schedule your HPV test appointment 2 weeks after the start of your menstrual period, up to about a week before your next menstrual period is due. This is the ideal time to have a HPV test when the clearest, cleanest sample of cervical cells can be obtained.
If you have reached menopause, you may schedule a HPV test at any time of the month.
Things to avoid:
48 hours before your Pap test, please avoid:
- douching
- swimming
- taking a tub bath
- sexual intercourse
- lubricants
- spermicides
- vaginal creams
- vaginal medications
- tampons
These activities or products can irritate the cervix. Avoiding these activities will help ensure adequate cell sample collection. Other factors that may affect HPV test results include infection and the intake of medication such as digitalis and tetracycline.
What To Wear For Your Appointment
For your HPV test appointment, please wear a two-piece outfit.
It may also be a good idea to bring along a panty liner or thin sanitary pad as light bleeding or spotting may occur after a HPV test.
Screen at SCS Clinic @ Bishan
SCS Clinic @ Bishan offer Pap Test and HPV Test screenings at no cost for eligible individuals. Our team will contact you within 5 working days to schedule an appointment, subject to availability.
Detailed Eligibility Criteria for Pap Test:
- Women aged 25 to 29
- Have had sexual activities
- Have not undergone a Pap test in the last 3 years
Detailed Eligibility Criteria for HPV Test:
- Women aged 30 and above
- Have had sexual activities
- Have not undergone a HPV test in the last 5 years
Human Papillomavirus (HPV) Vaccination
Apart from going for regular screenings, you can also reduce your cervical cancer risk by getting your HPV vaccination. The HPV vaccination can protect you against high-risk types of HPV, a virus that can lead to cervical cancer.
What is Human Papillomavirus (HPV)?
Human papillomavirus (HPV) is a group of common viruses that cause infections in both men and women. It is estimated that 8 out of 10 people will get HPV at some point in their lifetime. Most HPV infections clear up on their own and do not cause any problems. However, persistent infection by certain HPV types can cause cancer and other diseases over time.
HPV infection can cause several cancers. Virtually all cervical cancer cases (99%) are linked to genital infection with HPV. HPV can also cause other cancers such as anal cancer, mouth cancer, throat cancer, vaginal cancer, vulvar cancers and penile cancer.
HPV infection has no treatment or cure. The best way to help prevent HPV infection is to get vaccinated.
About the HPV vaccines
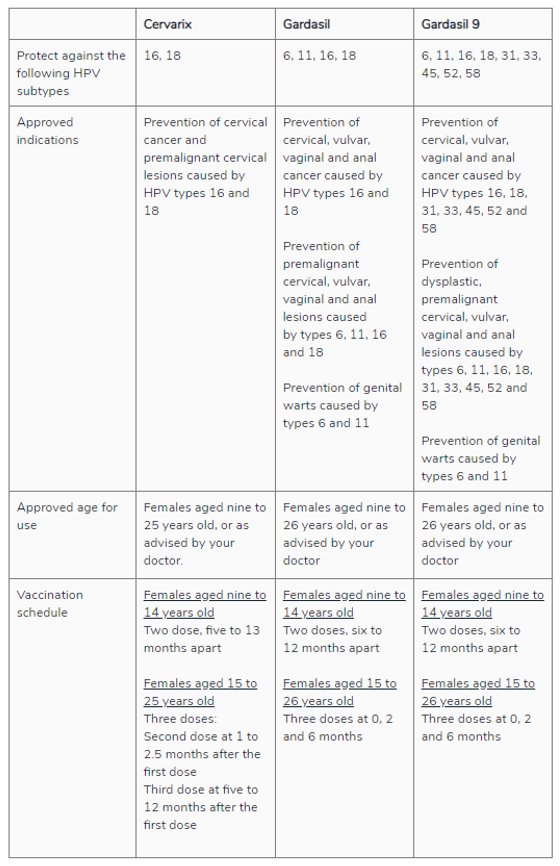
The vaccines approved for use in Singapore are Gardasil and Cervarix. The characteristics of the three vaccines are shown in the table below.
Where can I get vaccinated?
You can get your HPV vaccination at a polyclinic or GP clinic. It is advisable for you to consult your doctor to find out more before going for your HPV vaccination.
Singaporeans can also use up to $500 per Medisave account per year under the Medisave scheme to pay for HPV vaccination. They can use either their own or their immediate family member's Medisave (e.g. parents or spouse) to help pay for the vaccination.
The national school-based HPV vaccination programme
Health Promotion Board (HPB) offers the HPV Vaccination in secondary schools as part of the school-based vaccination programme. Parents of Secondary 1 female students (i.e. 12 to 13 years of age) who are eligible for the programme will be sent a consent letter, and HPB will work with the respective schools to schedule the HPV vaccination. Please refer to the fact sheet here.
For more information on the school-based HPV vaccination programme, parents can email [email protected] or call 6435 3895.
HPV Immunisation Programme
Ladies, have you had your Human Papillomavirus (HPV) vaccine?
Singapore Cancer Society (SCS) and Temasek Foundation are introducing a HPV Immunisation Programme to educate ladies on cervical cancer and the importance of HPV vaccination. As part of the programme, Temasek Foundation will fully fund the out-of-pocket cost of up to $23 per actualised dose of the HPV vaccination* for eligible ladies with SCS implementing the programme.
Cervical cancer is the 10th most common cancer affecting women in Singapore despite being one of the most preventable cancers. The HPV vaccination prevents specific types of HPV infections that may lead to cervical cancer and is key in cervical cancer prevention especially for young ladies before their first sexual exposure.
Hurry and complete your doses by 30 June before the programme reaches its natural conclusion!
*HPV 2 (Cervarix) is the only vaccine used in the HPV Immunisation Programme.
Check Your Eligibility:
The HPV vaccination is available at participating Community Health Assist Scheme (CHAS) General Practitioner clinics for Singaporean women aged 18 – 26 years old who holds a valid CHAS orange or blue card.
For eligible Singapore Citizens who are Green and non-CHAS Card holders, the maximum amount to be paid for the vaccination is $45 per dose. MediSave can be used to cover this out-of-pocket costs.
Eligible PRs will be able to enjoy subsidies at polyclinics only.


If you have already received your first dose of the HPV vaccination before 26 years old and have yet to receive your remaining two doses, please check with your doctor before making an appointment for the vaccination.
Make an Appointment
If you are eligible, you may contact your nearest clinic directly to schedule an appointment.
Participating Clinics
Click on your following district area (North, South, East, West, Central) to view the list of participating clinics:
|
First two digits of postal code 42 to 52, 81 |
|
|
First two digits of postal code 11 to 13 and 60 to 68 |
|
|
First two digits of postal code 1 to 10, 14 to 41, 58, 59, 77, 78 |
|
|
First two digits of postal code 69 to 73, 75 and 76 |
|
|
First two digits of postal code 53 to 57, 79, 80 and 82 |
Protect yourself against HPV and cervical cancer. Book your appointment for the Human Papillomavirus (HPV) vaccination today. Together we can beat HPV and cervical cancer!
FAQS
Who is at risk of HPV infection?
HPV is a common skin infection. Most people infected by genital HPV have no clear history of contact. However, the risk of infection is higher for individuals with:
Multiple sexual partners: The greater the number of sexual partners, the higher is your risk of HPV infection. Having sexual activity with a partner who has had multiple sex partners can also increase your risk. While using condoms can help reduce the risk of HPV infection, it does not cover all genital skin nor guarantees 100% protection.
Weakened immune system: People with weakened immune systems (e.g. may be due to Human Immunodeficiency Virus (HIV) / Acquired Immune Deficiency Syndrome (AIDS) or on immune-system suppressing drugs) are at higher risk of HPV infection.
How is HPV transmitted?
- HPV infection is very common in men and women
- It can be transmitted through genital skin-to-skin contact during sexual activity, by sharing contaminated sex toys and very rarely, during delivery from the infected mother to the baby.
- HPV cannot be passed by sitting on toilet seats or touching the door knobs
What are the signs or symptoms of HPV infection?
- Some HPV infections may cause genital warts
- High-risk HPV infection of the cervix does not cause any signs and symptoms. The abnormality on the cervix is detectable by cervical screening (Pap smear test) and by specific HPV test.
Can HPV be treated?
- The virus itself cannot be treated. Most HPV infections (90% of the cases) go away on its own without any treatment
- Although HPV virus cannot be treated, regular Pap smear can help to detect changes in the cervical cells caused by HPV infection
- With appropriate treatment, the abnormal or pre-cancerous cells can be prevented from developing into cervical cancer
I have a young daughter. Should she be vaccinated?
- The vaccine is approved for females aged 9 years to 26 years (depending on the specific vaccine being administered)
- The vaccines are most effective in protecting against the selected HPV sub-types if given before your daughter is exposed to them (usually through sexual activity)
- It is advisable to speak to your doctor to find out more about HPV vaccination
- Once you have understood the benefits, risks and limitations of the vaccines, the decision to proceed with vaccination is a personal one
Are the vaccines safe and effective?
- The two vaccines have been approved as safe and effective
- Long-term safety and efficacy are still under evaluation
- The vaccines consist of neither the viruses nor any infectious material. This means you cannot get HPV infection from the vaccines
Are HPV vaccines 100% effective in preventing cervical cancer?
- No. As with any vaccination, HPV vaccinations do not guarantee 100% protection
- HPV vaccinations are not substitutes for routine cervical cancer screening
- Women who received vaccination are still encouraged to continue going for Pap smear once every three years
Should my son go for HPV vaccination?
- Currently the National Childhood Immunisation Schedule (NCIS) only includes HPV vaccination for females aged 9 to 26 years old
- The decision to proceed with vaccination is a personal choice
- We advise you to speak to your doctor to find out more about the benefits and limitations of vaccinating your son against HPV